Overview
Spinal decompression can be performed via multiple techniques commonly used. Common performed techniques include Superion Vertiflex and Vertos Minimally Invasive Spine Decompression (MILD procedure). These procedures are intended to provide additional space for nerves compressed by spinal stenosis. Direct decompression typically involves removing the structure which is compressing the nerves. This structure is typically the ligamentum flavum. MILD is an example of direct decompression. Indirect compression typically uses a small medical device to open up the spinal canal. Superion Vertiflex is an example of indirect decompression. Your physician can better discuss what is the best option for you.
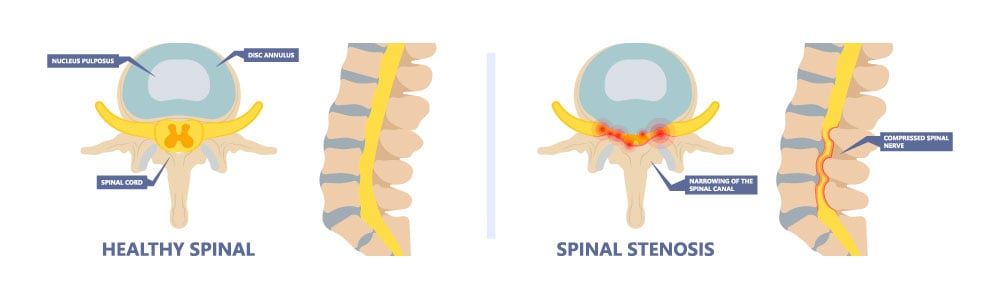
What conditions are treated with spinal decompression?
Direct and/or indirect spinal decompression techniques are used for the treatment of spinal stenosis. Patients who suffer from spinal stenosis typically have symptoms of back pain, leg pain, leg weakness, and/or leg cramping. These symptoms are made worse with walking; this is known as neurogenic claudication. Symptoms typically improve with rest and mildly bending forward. Patients oftentimes can consider surgical decompression known as laminectomy. Direct or indirect spinal decompression is a minimally invasive approach commonly used for patients who are trying to delay surgery or cannot have surgery due to their other medical conditions.
How is the procedure performed?
Our team will help position you to make sure the procedure can be completed with the least amount of discomfort for you. The skin is cleansed with a sterilizing solution (chlorhexidine) and a sterile drape is placed. A local anesthetic medication typically (Lidocaine) is given to numb the skin. Next, fluoroscopy (x-ray) or ultrasound is used to find the target. Next depending on the technique used a small device is used to open up the spinal canal. Your physician can discuss this more in detail before the procedure. During the entire procedure you will be constantly monitored by our team. After the injection a small bandage is placed on your skin. You will be given time after the procedure to make sure you feel good and are not having side-effects before leaving the clinic.
Does the procedure hurt?
The procedure is typically well tolerated. A localized burning sensation from the anesthetic is commonly felt and is usually the most uncomfortable part of the process. During the procedure a pressure sensation is often experienced this typically resolves within a few minutes. Minor soreness for a week after the procedure is normal.
How long does the procedure take?
The procedure typically takes about 1 hour to perform. Please plan on being at the surgery center or hospital for about 3-4 hour to allow for pre- and post-procedural safety protocols.
How quickly will I get relief?
Relief should start within 1 week.
How long can I expect the relief to last?
Every patient is different. Our goal is for you to get long-term relief from the decompression procedure.
How often can the procedure be repeated?
The procedure typically does not need to be repeated. However, if you have multiple areas of spinal stenosis the procedure could be considered at other locations.
What are the risks and side effects?
Risks and side effects are minimal and serious complications are rare. We take every precaution to ensure safety. Potential risks may include but are not limited to: vasovagal response (passing out), new or increased pain, bone fracture, infection, bleeding, permanent skin changes, allergic or unexpected drug reaction with minor or major consequences, and unintended nerve injury.
Pre-Procedure Information
Please let us know if you have an active infection, are using antibiotics, or are using blood thinners.
Should I take my normal medications as scheduled?
Yes. Continue taking your prescribed medications prior to procedure.
What if I am on a blood thinner or Aspirin?
Anticoagulation is often stopped for a short period of time prior to injection. Please speak with your primary physician if you take blood thinners to make sure that you can safely stop taking these medications.
Do I need a driver?
Yes. For your safety we require a driver to ensure a safe return home.
Can I eat the day of the procedure?
You must fast for at least 8 hours prior to the procedure. Do not eat after midnight the night before the procedure.
Can I get sedation or anesthesia?
IV anesthesia is provided. A breathing tube is typically not needed. The anesthesia level is similar to that of a colonoscopy.
What if I am pregnant?
There are serious potential risks to an unborn fetus when exposed to imaging studies, including x-ray and fluoroscopy. If there is any chance you may be pregnant, please postpone this procedure until it can be confirmed that you are not pregnant as it is not safe to do during pregnancy.
What should I wear?
We recommend light loose-fitting clothes. Sometimes we will ask you to change into a gown.
Post-Procedure Information
When can I drive after the procedure?
We recommend resuming driving in about 1 week.
What can I do if I am sore or have pain after the procedure?
Ice packs can be applied to the area for 20 minutes per hour. Over the counter Tylenol and Motrin can be used to aid with any discomfort.
What are my restrictions after the procedure?
Typically, you may resume light activities on the same day following your procedure. Physical therapy can be re-started within 24 hours. We recommend returning to work the day after the procedure.
When can I shower?
Showering the day of the procedure is allowed. For 24 hours you are asked to refrain from submerging or swimming in water. Keep the bandage on for one day.
When do I come back for a follow-up visit?
We follow-up with all of our patients after their procedures. We typically see patients back in 2 weeks.
